Reproductive Rights in Irish Law: A Beginner’s Guide
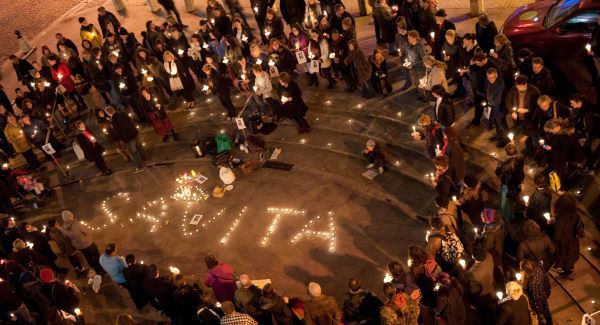
When the tragic news of Savita Halappanavar’s death was circulated around the world on Wednesday, it brought Ireland’s strict anti-abortion laws to international public attention. Many people have been shocked to learn that a European country has such a conservative approach to reproductive rights, and are unaware of how much more restrictive Ireland’s laws were in the recent past. Over the past few years, I’ve learned a lot about this issue from Irish friends and visiting activists, and this is my attempt to collect as much of that information as possible into a single blog post.
Ireland formally became independent from the UK in 1922, so the early laws forbidding abortion come from English law; specifically the Offences Against The Person Act, 1861 which made abortion punishable by a life sentence. Although the ban on abortion was superseded in England and Wales by the 1967 Abortion Act, the offence is still on the statutes in both the Republic of Ireland and Northern Ireland.
For much of the Twentieth Century, it was difficult to obtain any form of contraception in Ireland, or even to find information about it. The 1929 Censorship of Publications Act, made it illegal to print or distribute any publication which “advocate[d]… the unnatural prevention of conception or the procurement of abortion or miscarriage or any method, treatment, or appliance to be used for the purpose of such prevention or such procurement”. However, the increasing industrial production of condoms in the 1930s meant that it was no longer sufficient just to ban anyone from writing about them, so the Irish government, then led by Eamon de Valera, banned the sale or import of contraceptives under the Criminal Law Amendment Act, 1935. The ban was rooted in Catholic sexual morality, but there are also suggestions that it was influenced by a perceived need to maintain population levels during a period of mass emigration.
Crucially, the 1935 Act didn’t make it a criminal offence to possess contraceptives, just to exchange them for money. Some people visited family planning centres which gave away condoms as a “gift” to anyone who made a donation, while others got their supplies on trips to Northern Ireland or other parts of the UK, where condoms could be bought over the counter from a pharmacist. Some women even managed to get the contraceptive pill, either on the black market, or by persuading their doctor that they had sufficiently irregular or painful periods to justify being prescribed it on medical grounds.
In May 1971, members of Irish Women’s Liberation Group took the famous Contraceptive Train to Belfast, and challenged the legal status quo by purchasing large quantities of condoms, spermicides and diaphragms, and openly declaring their purchases at Customs on their return (they faced no criminal charges, mainly because the customs officers were too embarrassed to stop them). By this point, opinions in the Irish government and legal system were beginning to shift; in 1973 the Supreme Court ruled that it was unconstitutional to ban the import of condoms for personal use, and while it remained illegal to sell them, there are anecdotal accounts suggesting that the police turned a blind eye – sometimes because they were using the same illicit condom dealers as everyone else.
During this period there was also public opposition towards any form of birth control, including amongst certain sections of the medical community. From the 1940s until perhaps as recently as the early 1990s, some doctors in Ireland were still using a procedure known as a symphysiotomy, where the patient’s pelvis is surgically widened by the cutting ligaments holding the symphysis together, as an alternative to the caesarian section, even though it caused chronic pain, mobility problems, and incontinence. C-sections were believed by some doctors to encourage contraception, as there is a limit to the number of times that a woman can undergo the operation before further pregnancies become unsafe, whereas a symphysiotomy didn’t limit the number of future pregnancies. Although symphysiotomies were relatively rare, the few doctors who used the procedure didn’t obtain informed consent, and instead went ahead without properly explaining the risks and alternatives.
It was only in 1980, with the commencement of the Health (Family Planning) Act, that it finally became legal to obtain contraception in the Republic of Ireland, although only with a prescription, and either the doctor or pharmacist could refuse to provide them on the grounds of religious objection. Technically, anyone could ask for contraceptives, but in practice it could be difficult to get a prescription unless you were married. In 1985 the Act was amended to allow over-the-counter sales.
But while the trend towards liberalising the laws on contraceptive access continued, the legal barriers to abortion were strengthened. In 1983, an amendment was added to the Irish constitution giving a foetus an equal right to life as the woman gestating it (similar to some of the “foetal personhood” laws proposed in the US over the last few years), although it potentially allows an abortion to be carried out when it is the only way to save the woman’s life. As part of the constitution, it can only be changed by a referendum – essentially, Irish law was abortion-proofed to make it impossible for any future government to change the law while a large section of the population are strongly opposed.
Since abortion was legalised in England, Scotland and Wales in 1968, some Irish women have been able to travel to the UK to have the procedure, usually in London or Liverpool, but this solution is far from ideal. It’s not cheap – on top of travel costs, they have to pay the fees at a private clinic – and there are often logistical issues, like getting time off work or arranging childcare, which can be difficult if you can’t be open about why you need to go away for a few days (remember that institutions like the Magdalene Asylums were around until the 1990s). In addition, censorship laws meant that until 1995 it was illegal to give a woman information about how to go about arranging an abortion in England, so the phone numbers for clinics or support groups in the UK had to passed around in secret. In spite of this, thousands of women would make the trip across the Irish Sea to get their abortion every year.
But even the right to have an abortion abroad has been called into question, most famously in what is known as the X Case. X was a 14-year-old girl who had become pregnant after being raped by a friend of the family, who was later discovered to have been sexually abusing her for a number of years. She decided to have an abortion, so her parents made arrangements to take her to London, but also contacted the Gardai to ask if it might help the investigation if the foetus could be tested for proof of paternity. The information about X’s planned abortion eventually reached the Attorney General, who issued an injunction to stop her from leaving the country, citing 1983 constitutional amendment, which gave the foetus equal rights to X. Although X was already in London by this point, she and her parents had to return to Ireland until her fate could be decided by the courts. After a month of court cases and appeals, X was finally given permission to leave Ireland to have an abortion on the grounds that the pregnancy was endangering her life by making her suicidally depressed, but she had a miscarriage before arriving for her appointment.
The X case sparked a wave of pro-choice protests in Dublin, and a referendum, where the Irish public voted on three separate constitutional amendments: the right to travel without limitation, the right to information about abortion services legally available in other countries, and that a serious risk of suicide should not be considered as a life-threatening condition when deciding whether a woman can have an abortion in Ireland. The first two amendments passed, meaning that women have the right to travel and receive information, while the third was rejected.
Despite the fact that the law theoretically allows doctors to carry out an abortion to save a woman’s life, there hasn’t been any specific legislation since the referendum to clarify exactly when abortion is acceptable, so in reality, most doctors are extremely reluctant to allow it. In 2010, the A, B and C v Ireland case in the European Court of Human Rights, three anonymous case studies were presented as examples of women who had suffered as a result of being unable to obtain an abortion or appropriate aftercare in their home country. Although A and B’s cases were dismissed, the ECHR found that C’s human rights had been breached, because she suffered from a rare form of cancer and it was unclear how pregnancy would affect her prognosis. Seven years later, there is still no clarifying legislation.
Before this week, much of the recent campaigning has centred around cases of women who have been told that the foetus they are carrying a foetus with severe abnormalities. Earlier this year the Termination for Medical Reasons campaign was launched by a group of women who had been forced to travel to England for a termination, because they felt unable to continue the pregnancy knowing that their baby would be stillborn, or only live for a very short time outside of the womb. This is a landmark campaign because several of the women involved have decided not to conceal their identities, instead openly admitting that they have terminated a pregnancy, and offering their experiences as case studies.
Although there appears to be growing support for abortion rights in Ireland, particularly in cases of severe foetal abnormality, the are parts of society – and even the medical establishment – who still believe that abortion is never justified. In September this year, a medical conference in Dublin concluded that “direct abortion is not medically necessary to save the life of a woman”. Sadly, they’ve just been proved wrong by a woman in Galway.




Always follow your prescribed medications or
suffer from the annoying noise. For more information, just visit Tinnitus Cure Revealed dot Info.
Tinnitus maskers do not treat the condition except to drown out the ringing so that that a sufferer can function without being consumed by the noise.